Summary:
How Spinal Decompression Works to Relieve Disc Pressure
Spinal decompression uses controlled mechanical traction to gently stretch your spine. That stretch creates negative pressure inside your discs—think of it like a vacuum effect that can reach as low as -110 mm Hg according to clinical measurements.
Why does that matter? Because that negative pressure does two things traditional treatments can’t. First, it encourages herniated or bulging disc material to retract back toward the center where it belongs. Second, it allows oxygen, water, and nutrients to flow back into degenerated discs, supporting the healing process your body wants to do naturally.
The computerized systems used today bypass your body’s protective muscle guarding response. When you manually pull on someone’s spine, muscles tighten up to protect you—that’s the proprioceptor response. Modern decompression tables apply force slowly and rhythmically, cycling between stretch and relaxation, so your muscles don’t fight the treatment. That’s the key difference between this and older traction methods that just pulled without that sophisticated control.
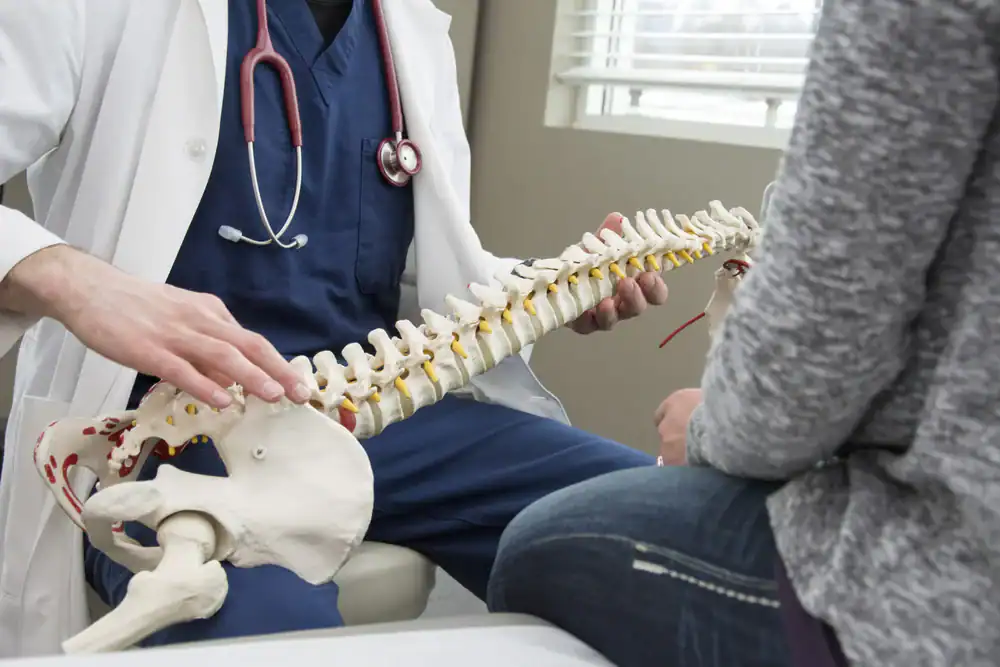
What Does Spinal Decompression Feel Like During Treatment
Most people expect discomfort. What they actually experience is closer to a gentle, elongating stretch—the kind that makes you want to close your eyes and breathe deeper.
You’ll lie on a specialized table, secured with soft harnesses around your pelvis and torso. The table slowly applies traction for 20-30 minutes, alternating between periods of gentle pulling and relaxation. Many patients describe it as feeling like someone’s carefully lifting weight off their back. Some people fall asleep during sessions because the sensation is that calming.
The first week or two, you might feel a dull, achy soreness—similar to how your muscles feel after trying a new workout. That’s your body adjusting to the realignment and decompression. It’s not sharp pain. It’s not nerve pain shooting down your leg. It’s the kind of soreness that tells you something is changing.
By the third or fourth session, most people notice that soreness fades and the relief becomes more obvious. You might notice you can sit longer without pain. Or that the tingling in your leg has decreased. Or that you’re standing straighter without thinking about it.
Some patients feel improvement after just one session. Others need six to eight sessions before they notice significant change. Around 80% of patients experience meaningful relief when they complete the full treatment protocol, which typically runs 12-20 sessions over four to six weeks. About 20% see relief in the first week. Another 40% feel significant improvement by weeks two or three. The remaining 20% who respond well get their relief between weeks four and six.
Spinal Decompression vs Traditional Traction Therapy
Traction has been around for decades. It’s simple: apply a pulling force to create space between vertebrae. Manual traction uses a therapist’s hands. Mechanical traction uses pulleys, ropes, or harnesses. Both can provide temporary relief for mild discomfort, but they lack precision.
Traditional traction applies static or constant force. Your body senses that pull and often responds with muscle spasms or guarding. The force isn’t targeted to specific disc levels, so you’re stretching everything rather than focusing on the problem area. Results tend to be short-term because you’re not creating the negative intradiscal pressure needed for actual disc healing.
Spinal decompression is different. It uses computer-controlled tables that monitor your body’s response hundreds of times per second. The system adjusts the angle, intensity, and duration of the pull based on real-time feedback. This precision allows the therapy to target specific discs—L4-L5, L5-S1, or cervical levels—rather than just generally stretching your spine.
The research backs up the difference. One study comparing decompression to standard traction found that 86% of ruptured disc patients had good-to-excellent results with decompression compared to 55% with traction. Fluoroscopic imaging confirmed up to 7mm of vertebral separation at L5 during decompression treatment. That’s measurable space that allows discs to decompress and heal.
Traction can help with muscle spasms or mild spinal stenosis. Decompression is better suited for moderate to severe disc conditions—herniations, bulges, degenerative disc disease, and nerve compression causing sciatica. If you’ve tried traction without lasting results, decompression may be the next logical step before considering surgery.
Want live answers?
Connect with a DR Roses expert for fast, friendly support.
Who Benefits Most from Spinal Traction Therapy
Not everyone needs spinal decompression. But if you’re dealing with specific disc-related issues that haven’t responded to basic conservative care, you might be an ideal candidate.
People with herniated or bulging discs often see the most dramatic results. When disc material presses on nerve roots, you get radiating pain—sciatica down the leg, or pain shooting into your arm from cervical issues. Decompression can retract that herniated material and relieve the nerve pressure causing your symptoms.
Degenerative disc disease is another strong indication. As discs lose height and hydration over time, they can’t absorb shock the way they should. The negative pressure created during decompression helps rehydrate those discs, bringing in nutrients and improving their function. Studies show about 70% of degenerative disc patients report reduced pain with this approach.
Spinal stenosis—narrowing of the spinal canal that compresses nerves—also responds well. Research indicates 75% success rates for stenosis patients using decompression, which compares favorably to surgery’s 10-15% failure rate.
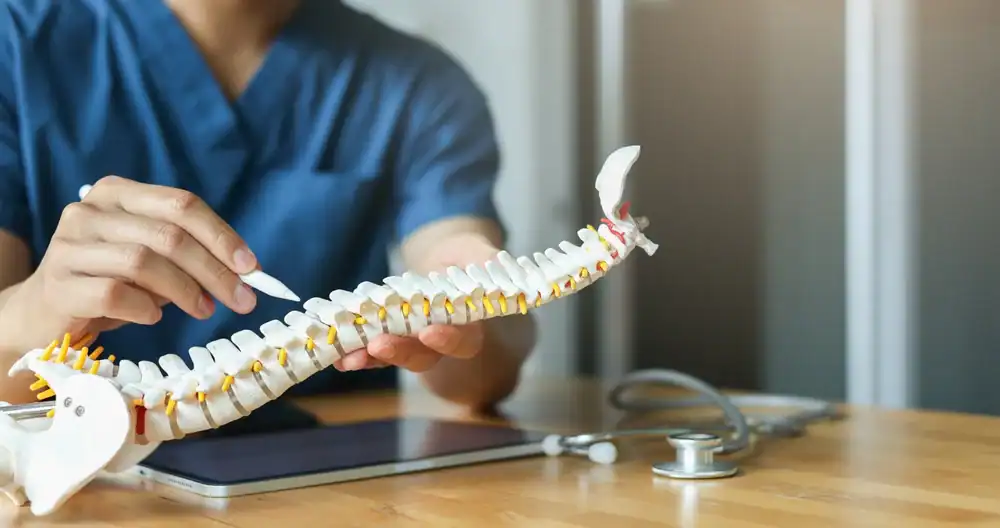
When Spinal Decompression Is Used Instead of Surgery
Surgery should never be your first option for disc problems unless you’re facing a true emergency—like cauda equina syndrome with loss of bowel or bladder control. For most people dealing with chronic back pain, herniated discs, or sciatica, conservative treatment makes sense to try first.
Here’s why that matters: spinal decompression costs between $1,290 and $3,900 for a full treatment course. Spinal surgery averages $50,000 or more, even with insurance. Recovery from surgery takes months. Recovery from decompression therapy? You can go back to work the same day.
The success rates are comparable. Non-surgical decompression shows 71-89% success rates for disc conditions. Spinal surgery reports 80-90% success rates, but 10-20% of patients experience complications or need revision surgery. Failed back surgery syndrome affects about 20% of surgical patients at an average of 3.4 years post-op.
Between 1990 and 2000, spinal fusion surgery increased by 220% despite no clear indication that it worked better than conservative care. Many surgeons now recommend trying decompression before even discussing surgical options. That’s not because surgery doesn’t work—it’s because for many patients, surgery is overkill when less invasive options can achieve similar results.
The best candidates for decompression are people who’ve had symptoms for weeks or months, have tried basic treatments like rest and physical therapy without complete relief, and want to avoid surgery if possible. You’re also a good fit if imaging shows a herniated disc, bulge, or degenerative changes that correlate with your symptoms.
You’re not a candidate if you have severe osteoporosis, spinal fractures, tumors, or certain types of spinal instability. Pregnancy is typically a contraindication for lumbar decompression, though some practices offer modified cervical traction for pregnant patients. We’ll review your history and imaging to determine if decompression is safe and appropriate for you.
What to Expect During a Spinal Decompression Treatment Plan
A typical treatment plan involves 12-20 sessions spread over four to six weeks. Sessions usually happen three to five times per week initially, then taper as you improve.
Your first visit includes a thorough evaluation. Expect a detailed health history, physical exam, and review of any imaging you’ve had—MRIs, X-rays, or CT scans. We also use infrared imaging to assess nerve function and inflammation patterns. This baseline helps track your progress objectively.
Each treatment session lasts about 30-45 minutes. You’ll lie comfortably on the decompression table while the system applies controlled traction. The table alternates between stretching and relaxation cycles, gradually building to a peak force calculated specifically for your body weight and condition. Most patients find it relaxing enough to read, listen to music, or even nap.
After each session, many people notice immediate changes—less pressure in the back, easier movement, reduced leg pain. Others experience more gradual improvement over multiple sessions. We’ll likely combine decompression with other therapies: corrective exercises to strengthen supporting muscles, ergonomic coaching to prevent re-injury, and possibly adjustments or soft tissue work.
Hydration matters during treatment. Drinking plenty of water helps your discs rehydrate more effectively. Light activity like walking supports recovery better than complete rest. Avoid heavy lifting or prolonged sitting immediately after sessions, and pay attention to your posture throughout the day.
Most people complete their initial treatment plan and then transition to maintenance care or periodic sessions as needed. Some need ongoing support every few weeks or months. Others find that once they’ve achieved relief, they can maintain it with exercise and lifestyle modifications alone.
The key is consistency. Missing sessions or stopping treatment early reduces your chances of long-term success. Think of it like physical therapy—you get out what you put in.
Is Spinal Decompression Right for Your Back Pain
Spinal traction and decompression therapy aren’t miracle cures, but they’re proven options that help the majority of people avoid surgery. The treatment creates measurable changes in disc pressure, promotes natural healing, and comes with minimal risk compared to surgical intervention.
If you’re dealing with a herniated disc, sciatica, degenerative disc disease, or nerve compression that hasn’t responded to basic conservative care, decompression deserves consideration. The gentle stretching sensation, high success rates, and ability to return to normal activities immediately make it a practical choice for people who want relief without the cost and recovery time of surgery.
The decision comes down to where you are in your journey. If you’ve only tried rest and over-the-counter pain relievers, you might benefit from physical therapy or chiropractic adjustments first. If you’ve exhausted those options and surgery feels like the next step, decompression offers a middle ground worth exploring. For personalized guidance on whether spinal decompression fits your specific condition, reach out to us to discuss your options and get a thorough evaluation.