Summary:
What Is a Cervicogenic Headache
A cervicogenic headache is head pain that starts in your neck. The pain originates from structures in your cervical spine—the bones, joints, muscles, or nerves—and travels upward into your head. It’s referred pain, meaning you feel it in one place while the problem exists somewhere else.
These headaches typically affect one side of the head. The pain often begins at the base of the skull and moves forward toward the temple, forehead, or behind the eye. Unlike migraines, cervicogenic headaches don’t usually come with nausea or extreme light sensitivity. Instead, they’re accompanied by neck stiffness, reduced range of motion, and pain that worsens with certain head or neck positions.
The reason your neck can cause head pain comes down to anatomy. The upper cervical nerves share pathways with nerves that supply sensation to your head and face. When something irritates those cervical nerves—whether it’s a misaligned joint, tight muscle, or compressed nerve root—the pain signal gets interpreted by your brain as coming from your head.

How Upper Neck Tension Creates Headache Patterns
Your upper cervical spine—specifically the top three vertebrae—plays an outsized role in headache development. These vertebrae (C1, C2, and C3) sit right at the junction where your skull meets your neck. They’re designed for mobility, allowing you to turn and tilt your head in multiple directions. But that mobility comes with vulnerability.
When the joints between these vertebrae become restricted or misaligned, they can irritate nearby nerves. The suboccipital muscles—small but powerful muscles at the base of your skull—often become tight and overworked when your neck alignment is off. These muscles connect directly to the dura mater, the membrane surrounding your brain and spinal cord. Tension here can trigger headache pain that feels deep and persistent.
Forward head posture is one of the biggest contributors to this problem. When your head juts forward—common when looking at screens, driving, or sitting at a desk—it adds significant weight and strain to your upper cervical spine. For every inch your head moves forward from neutral alignment, it effectively adds 10 pounds of force on your neck structures. Over time, this sustained pressure creates chronic muscle tension, joint dysfunction, and nerve irritation.
Poor sleeping positions compound the issue. If your pillow is too high, too flat, or doesn’t support the natural curve of your neck, you’re spending hours each night with your cervical spine in a compromised position. That’s why some people wake up with headaches or develop them shortly after getting out of bed.
Injuries also play a role. Whiplash from a car accident, a fall, or sports impact can damage the ligaments and soft tissues supporting your upper neck. Even after the acute injury heals, the altered mechanics can persist, creating a pattern of recurring cervicogenic headaches months or years later.
The key point: your neck position and alignment directly influence whether you develop headaches. Addressing the mechanical problem in your neck is often more effective than treating the head pain in isolation.
Common Triggers That Connect Neck Pain to Headaches
Certain activities and positions predictably trigger cervicogenic headaches. Recognizing your specific triggers helps you make adjustments before the headache starts.
Prolonged static positions top the list. Sitting at a computer for hours, especially with your monitor too low or too high, forces your neck into sustained flexion or extension. Your neck muscles aren’t designed to hold your head in one position for extended periods. They fatigue, tighten, and eventually refer pain into your head. The same thing happens during long drives, extended phone use with your head tilted down, or any activity that keeps your neck locked in place.
Repetitive head movements create similar problems through a different mechanism. Jobs that require frequent turning—like hairstylists, truck drivers checking mirrors, or workers on assembly lines—can overwork specific neck muscles and joints. The repetitive stress accumulates, leading to inflammation and irritation in the cervical structures.
Stress and muscle tension form a vicious cycle with cervicogenic headaches. When you’re stressed, you unconsciously tighten your neck and shoulder muscles. That tension restricts blood flow, creates trigger points, and pulls on the joints of your upper cervical spine. The resulting headache then increases your stress level, which tightens the muscles further.
Physical strain matters too. Lifting heavy objects with poor form, carrying a heavy bag on one shoulder, or sleeping on your stomach with your head turned to the side all place abnormal forces on your neck. These forces can shift vertebrae out of optimal alignment or strain the muscles and ligaments that stabilize your cervical spine.
Temperature and environmental factors sometimes play a role. Cold drafts hitting your neck—from air conditioning vents, open car windows, or fans—can cause protective muscle spasms that trigger headaches. Similarly, sudden movements like jerking your head to look at something quickly can irritate already-sensitized cervical structures.
Understanding your personal trigger patterns allows you to make targeted changes. If you notice headaches consistently developing after certain activities or positions, that’s valuable information pointing you toward both prevention strategies and the likely source of your problem.
Want live answers?
Connect with a DR Roses expert for fast, friendly support.
Practical Home Strategies for Neck-Related Headaches
You don’t have to wait for professional treatment to start addressing cervicogenic headaches. Several practical strategies can reduce the frequency and intensity of neck-related head pain when applied consistently.
Posture awareness and correction form the foundation. Start by evaluating your typical sitting position. Your ears should align over your shoulders, not jutting forward. Your shoulders should be relaxed, not hunched or rounded forward. Your computer monitor should be at eye level so you’re looking straight ahead, not down or up. Making these adjustments reduces the sustained strain on your upper cervical spine.
Simple stretches and movements throughout the day prevent muscles from locking into tension patterns. Gentle neck rotations, side bends, and chin tucks help maintain mobility in your cervical joints and release building tension before it triggers a headache. The key is frequency—doing these movements for 30 seconds every hour is more effective than one longer session at the end of the day.
Your sleeping setup deserves attention. The right pillow supports the natural curve of your neck without pushing your head too far forward or letting it drop backward. Side sleepers generally need a thicker pillow than back sleepers. Stomach sleeping is problematic for neck health because it requires keeping your head turned to one side for hours, placing rotational stress on your upper cervical spine.

Ergonomic Adjustments That Reduce Neck Strain
Your work environment significantly impacts whether you develop cervicogenic headaches. Small ergonomic changes can eliminate many of the sustained positions and repetitive stresses that trigger neck-related head pain.
Start with your desk setup. Your chair height should allow your feet to rest flat on the floor with your knees at roughly 90 degrees. Your desk height should let your elbows rest at 90 degrees when your shoulders are relaxed. If your desk is too high, your shoulders hunch up. Too low, and you lean forward, both creating neck strain.
Monitor position is critical. The top of your screen should be at or slightly below eye level when you’re sitting with good posture. Position the monitor about an arm’s length away. If you’re constantly looking down at your screen, you’re spending hours in forward head posture, which overloads your upper cervical spine.
For laptop users, the built-in screen and keyboard create an impossible ergonomic situation—you can’t have both at optimal positions simultaneously. Use an external keyboard and mouse so you can elevate your laptop screen to proper height. Or use an external monitor and keep your laptop closed.
Phone use requires conscious adjustment. Holding your phone at chest level and looking down at it for extended periods is one of the worst positions for your neck. Bring the phone up to eye level instead. For longer calls, use speaker mode or headphones so you’re not cradling the phone between your ear and shoulder.
Driving posture matters too. Adjust your seat so you can reach the pedals comfortably without stretching. Position your rearview mirror so you have to sit with good posture to see it clearly—this creates a built-in reminder to maintain proper alignment. Adjust your side mirrors properly so you’re not constantly turning your head to check blind spots.
For people who read frequently, book stands or reading pillows can maintain better neck position than looking down at a book in your lap. The same principle applies to tablets—prop them at an angle that keeps your head in neutral position rather than flexed forward.
These adjustments might feel awkward initially because your body has adapted to poor positions. Give yourself a week or two to adjust. The reduction in neck tension and headaches makes the transition worthwhile.
When to Consider Professional Evaluation for Neck Alignment
Home strategies help many people reduce cervicogenic headaches, but some situations warrant professional evaluation. Knowing when to seek help prevents chronic problems from becoming entrenched patterns.
Consider professional evaluation if your headaches are becoming more frequent or intense despite your home efforts. Worsening patterns suggest an underlying mechanical problem that needs specific correction. Similarly, if your headaches are disrupting your work, sleep, or daily activities, you’re past the point where self-care alone is likely to resolve the issue.
Headaches that consistently occur on the same side of your head and are accompanied by neck pain or stiffness fit the classic cervicogenic pattern. These respond well to treatments that address the cervical spine directly. If you notice your headaches are triggered by specific neck movements or positions—turning your head, looking up, or maintaining certain postures—that’s another strong indicator that your neck mechanics need professional attention.
Recent injuries increase the likelihood that your headaches stem from cervical spine dysfunction. Whiplash from a car accident, a fall that jarred your neck, or a sports injury can create misalignments or soft tissue damage that won’t resolve on its own. Even if the injury happened months or years ago, it can create lasting changes in how your neck functions.
Limited neck range of motion alongside your headaches suggests joint restrictions or muscle tightness that needs hands-on treatment. If you can’t turn your head fully to one side, can’t tilt your head comfortably, or feel pulling or catching sensations with neck movement, those are mechanical problems that respond to specific interventions.
Headaches accompanied by arm pain, numbness, tingling, or weakness require prompt evaluation. These symptoms suggest nerve compression in your cervical spine that may need more aggressive treatment. Similarly, sudden severe headaches, headaches with fever, or headaches after head trauma need immediate medical attention to rule out serious conditions.
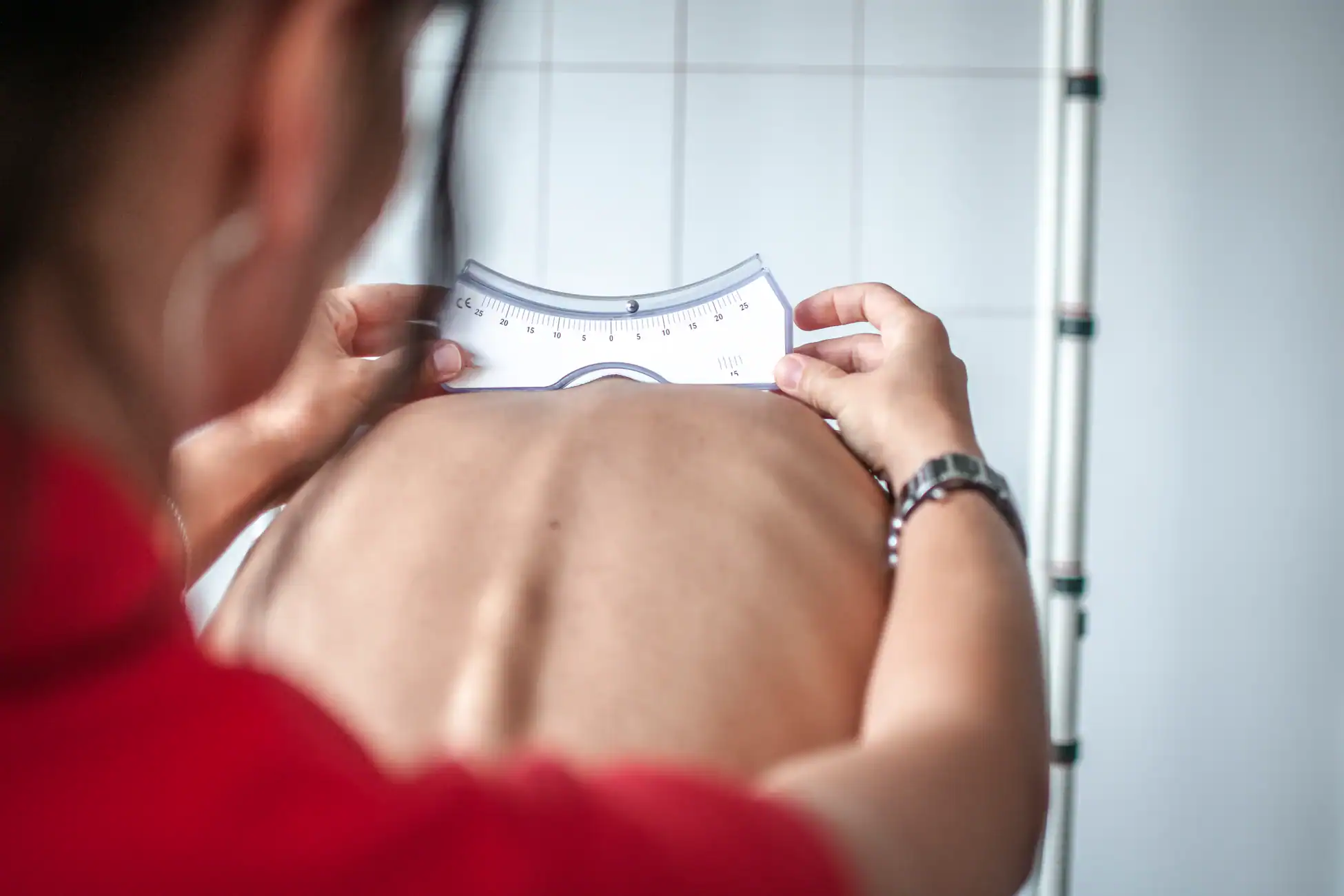
For Hudson County residents, chiropractic evaluation offers a non-invasive approach to diagnosing and treating cervicogenic headaches. Our evaluation typically includes a detailed history of your headache patterns, a physical examination of your neck mobility and alignment, and specific orthopedic tests to identify which cervical structures are involved.
Treatment for cervicogenic headaches focuses on restoring normal motion to restricted joints, releasing tight muscles, and correcting postural imbalances. Chiropractic adjustments to the upper cervical spine can reduce nerve irritation and improve joint function. Soft tissue techniques address muscle tension and trigger points. Exercise recommendations strengthen weak muscles and improve your ability to maintain proper neck alignment.
The goal isn’t just stopping your current headache—it’s correcting the underlying mechanical dysfunction so headaches don’t keep returning. That requires identifying the specific problem in your neck and applying targeted treatment to resolve it.
Many people wait months or years before seeking help for cervicogenic headaches, assuming they’ll eventually go away or that nothing can be done. The reality is that the sooner you address the mechanical problem in your neck, the easier it is to correct and the better your long-term outcome.
Finding Relief When Your Neck Is Causing Your Headaches
Headaches that originate in your neck respond differently than other types of head pain. Understanding the connection between upper cervical tension, posture, and headache patterns gives you a framework for addressing the real problem instead of just managing symptoms.
Start with the practical strategies you can implement immediately—improving your posture, adjusting your work environment, and being mindful of positions and activities that trigger your headaches. These changes reduce the daily strain on your neck and often decrease headache frequency.
When home strategies aren’t enough, or when your headaches are significantly impacting your life, professional evaluation makes sense. Cervicogenic headaches are mechanical problems that respond well to treatments addressing the cervical spine directly.
If you’re in Hudson County and dealing with persistent headaches accompanied by neck pain or stiffness, we’ve been helping local residents identify and treat the neck-related causes of head pain for over 30 years. Understanding what’s actually causing your headaches is the first step toward lasting relief.